|
It has not spread to lymph nodes or distant sites. In some cases, it may have moved into the body of the uterus, but it has not progressed outside of the uterus. Stage 1 cervical cancerĪt stage 1, cancer has grown past the surface of the cervix to deeper layers of tissue. When cancerous cells are detected at this early stage, they can generally be successfully destroyed with proper treatment. Stage 0 is also commonly called “carcinoma in situ.” This stage is sometimes considered “pre-cancer” because the abnormal cells are only at the surface layer of the cervix and have not moved into deeper layers of cells. Here are brief descriptions of the main FIGO cervical cancer stages: Stage 0 cervical cancer Stages 1 through 4 are further broken down with letters (for instance, stage 1A or 1B) based on the size of the cancer. The numbers are used to describe the cancer’s progression, with the lowest being the least advanced. How cervical cancer is stagedįIGO cervical cancer stages are numbered from 1 to 4, with stage 0 sometimes used to refer to abnormal cells that have not grown past the surface layer of the cervix. On average, Moffitt's cervical cancer treatment outcomes exceed 1.5 times the national average.īelow, we discuss cervical cancer staging systems as they relate to both treatment decisions and survival rates. Moreover, the survival rates for all cervical cancer stages are likely to improve as more innovative and effective treatments are developed. It’s important to remember that these rates are based on averages and do not consider specific data, such as the patient’s age, type of cervical cancer and overall health condition. The American Cancer Society uses the SEER database maintained by the National Cancer Institute to provide survival rate statistics for cervical cancer patients at each SEER stage. Distant – spread to nearby organs or more distant parts of the body.Regional – growth beyond the cervix and uterus to nearby lymph nodes.Localized – no spread outside of the cervix or uterus.Known as the Surveillance, Epidemiology, and End Results (SEER) staging system, this way of categorizing cervical cancer cases has only three stages based on how far the cancerous cells have spread: This system-which classifies cancer into one of four numbered stages-is based on clinical results such as physical exams and diagnostic testing, and the FIGO stage plays a big role in shaping the patient’s treatment plan.Ī different staging system is used for tracking cervical cancer survival rates. For staging cervical cancer, most doctors use the FIGO staging system, named for its developers at the International Federation of Gynecology and Obstetrics. Staging is important because it drives diagnosis, prognosis and treatment. The results are used to determine the size of any tumors, whether the cancer has invaded tissues in and around the cervix and whether it has spread to other areas of the body. Cancer can be staged through a combination of imaging, physical exams, biopsies, tissue diagnoses and sometimes surgery. 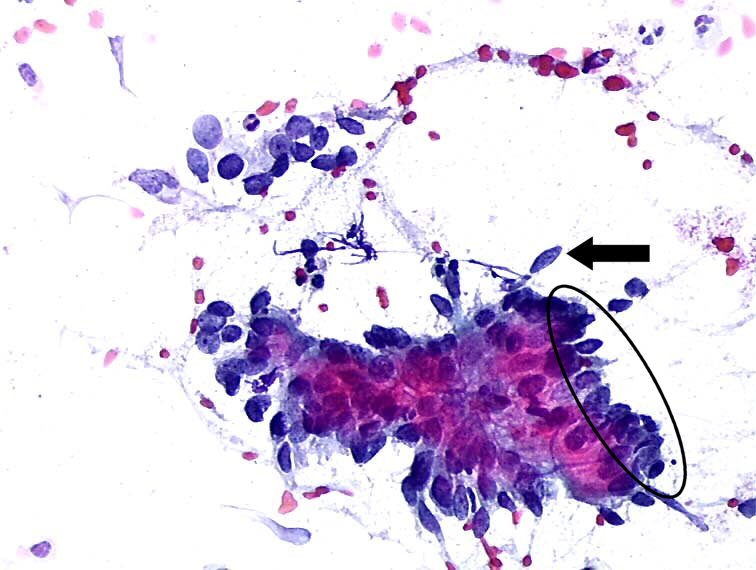
adenoma malignum: ~3% of adenocarcinomas 2Īdenocarcinomas in general (compared with squamous cell counterparts) are thought to generally give higher rates of thoracic and adrenal metastatic disease 1.Cervical cancer stages are identified with a complete clinical exam that is performed after a diagnosis is confirmed.endometrioid carcinoma of the cervix: ~7% of adenocarcinomas.There are several subtypes that fall under this category and include: Risk factorsĪside from smoking, cervical adenocarcinoma has the same risk factors as cervical SCC (see: cervical carcinoma for further details of risk factors) 6. They may arise from a precursor lesion, cervical adenocarcinoma in situ, and are almost always associated with HPV 18 5. PathologyĪs with squamous cell carcinomas, adenocarcinoma type also generally tend to arise from the squamocolumnar junction (SCJ). Cervical adenocarcinoma is less common than squamous cell carcinomas (SCC) of the cervix, accounting for ~12.5% of all cervical cancer. Their proportionate prevalence is thought to be increasing and this is thought to be due to being less readily detected by exfoliative cytology obtained with the Papanicolaou test 2-3.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
